CTC dysfunction was a leading non-infectious complication of this type of vascular access for haemodialysis 4, 5. After comparing dialysis patients from 20 countries, catheter usage ranged from 1% in Japan to 45% in Canada 3. The 2018 Annual Data Report of the United States Renal Data System (USRDS) showed that over 80% of the US patients started haemodialysis with a CTC, and in 69% of them the catheter was still in use after 90 days 2. It seemed to reduce fibrinolytic usage, allowed an immediate haemodialysis session commencement, therefore, it might save both the costs and the nursing staff time.Īccording to registries data, CTCs were used in 68% of the incident and 32% of the prevalent haemodialysis patients in Europe 1. 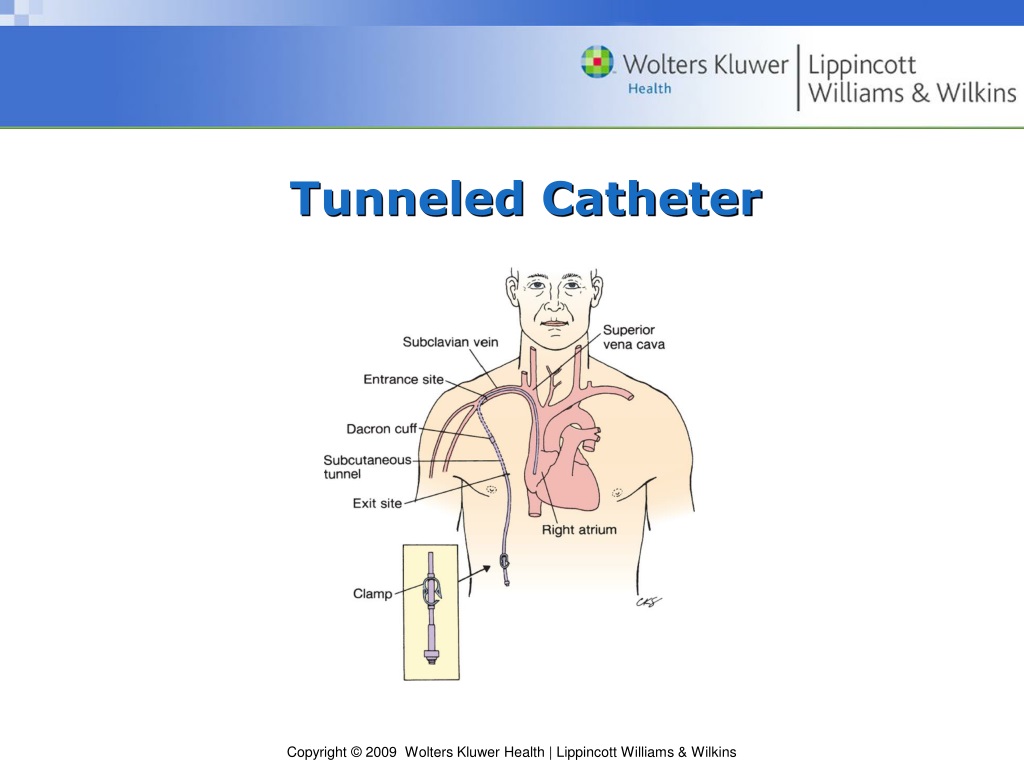
The novel NTCR manoeuvre was safe and effective in the majority of the CTC dysfunction episodes. Complications were observed only after 3.4% of all interventions. The procedure could be successfully repeated, with a similar result after the first and the second attempt. Overall, 86% of conducted NTCRs improved the CTC patency to perform a haemodialysis session. This study comprises the analysis of a total of 297 NTCRs, which were performed in 114 patients, thus enabling an effective blood flow after 133 procedures (44.7%).Partially effective blood flow followed 123 procedures (41.4%), and it failed altogether in 41 cases (13.9%). NTCR was based on gentle movements of the CTC, with or without a simultaneous flushing of the CTC lines, which resulted in a quick reposition of the CTC tip. 
The manoeuvre of a non-invasive tunnelled catheter reposition (NTCR) was introduced to restore the CTC function. However, all of them are time- and cost-consuming. When the CTC blood flow becomes ineffective, a number of protocols are advised. Despite all efforts, still many end-stage kidney disease (ESKD) patients are dialysed using a central tunnelled catheter (CTC) as vascular access.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
